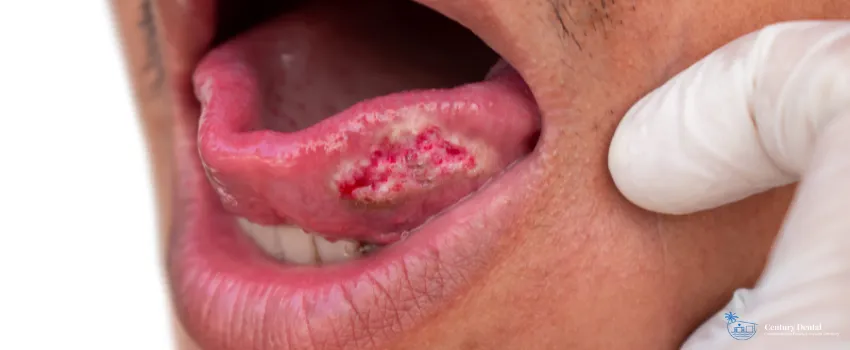
Oral cancer surgery is a critical step in treating this life-threatening disease. This blog explores the different options, success rates, and recovery processes for undergoing oral cancer surgery.
Oral cancer is a serious global health issue affecting many people. It’s about abnormal cell growth in the mouth, throat, tongue, or lips, which can harm our health. While there are different ways to treat it, oral cancer surgery is often a powerful option, especially when the cancer is in one place.
To show how urgent it is to learn about this, consider this: In 2018, there were about 354,900 new cases of oral cancer worldwide. Shockingly, 90% of these cases were a type called oral squamous cell carcinomas (OSCCs).
In this blog, we’ll dig deeper into oral cancer treatment, focusing on the role of surgery in fighting this severe disease.
Oral Cancer Surgery: Is it Right for You?
Oral cancer surgery is a potent treatment modality, but it’s imperative to ascertain its alignment with your unique health scenario. Here are some pivotal considerations:
1. Cancer Stage
Your oral cancer progression is instrumental in determining the surgical approach. Early-stage cancers, which haven’t metastasized, often witness higher surgical success rates.
2. Health Overview
A holistic assessment of your health and medical antecedents is vital. Your medical team will gauge your surgical fitness and the potential for a robust recovery.
3. Tumor Positioning
The tumor’s locale within the oral cavity can dictate the surgical strategy and its impact on daily functionalities.
4. Treatment Objectives
Engage in a comprehensive dialogue about your treatment aspirations with your healthcare provider. Surgery might be a component of a more extensive treatment regimen, potentially encompassing radiation or chemotherapy.
5. Potential Hazards
Grasping the potential risks and complications linked to surgery is crucial. The latter part of this blog will discuss the risk factors for post-operative complications in primary oral cavity cancer surgery.
6. Recovery Dedication
A steadfast commitment to post-operative care and consistent follow-up consultations is pivotal for optimal outcomes.
Transparent consultations with your healthcare professionals will empower you to make a well-informed decision about the appropriateness of oral cancer surgery in your treatment trajectory.
Surgical Removal as a Treatment Option for Oral Cancer
Oral cancer is removable. The primary objective of oral cancer surgery is to eradicate the malignant cells and thwart the disease’s progression to other body regions. The efficacy of the surgical procedure is contingent upon several factors, including the stage of the cancer, its location, and the patient’s holistic health.
For those contemplating surgery for oral cavity cancer, it’s imperative to engage in a comprehensive dialogue with their surgeon or oncologist. This ensures a thorough understanding of the anticipated outcomes, potential side effects, and the overarching risks and benefits associated with the procedure.
Oral Cancer Surgery Success Rate
The success rate of oral cancer surgery is influenced by the stage of the cancer and the patient’s overall health. The paramount goal is the complete removal of the tumor. Typically, the success rate is more favorable for early-stage cancers that haven’t metastasized.
For instance, the five-year survival rate for patients diagnosed with early-stage oral cancer, where the tumor has been successfully excised, hovers around 80% to 90%. However, the prognosis can be less optimistic if the cancer has metastasized to nearby lymph nodes or other distant regions.
A study on oral squamous cell carcinoma, the most prevalent intraoral malignancy, indicated that aggressive primary resection combined with adjuvant treatment yielded survival rates that were slightly better than the 56% five-year survival rate reported for oral cancer in England in 2010.
Another study emphasized that tumor relapses are observed in 25–30% of early-stage oral cavity squamous cell carcinoma cases and 50–60% of advanced cases. Managing these relapsed tumors is challenging due to the resistant nature of the cancer cells.
Despite these challenges, surgical resection remains a primary treatment modality, offering the best survival benefits.
Types of Surgery Used in Oral Cancer Treatment
Oral cancer surgery is a procedure performed to remove cancerous tumors and affected tissues in the mouth. It is typically done by a skilled oral surgeon or an otolaryngologist (ear, nose, and throat specialist). The goal of this surgery is to eliminate the cancer cells and prevent the disease from spreading further.
There are several types of oral cancer surgery, and the specific procedure used depends on the location and stage of the cancer. Let’s take a closer look at each surgery for oral cancer:
1. Primary Tumor Excision
This is the predominant method for oral cancer treatment, especially in early-stage cases. The procedure entails the removal of the primary tumor along with a margin of surrounding healthy tissue. Such excisions are particularly effective when the tumor is localized and hasn’t metastasized.
2. Mohs Surgery
Known formally as Mohs micrographic surgery, this technique is renowned for its precision. The surgeon meticulously removes the tumor layer by layer, examining each under a microscope until no traces of cancer cells remain. It’s especially favored for oral cancers situated in areas where conserving tissue is paramount, like the lips and nose.
3. Neck Dissection
This surgical approach targets the removal of cancer-afflicted lymph nodes in the neck, a common metastasis site for oral cancer. Often, neck dissection is performed alongside primary tumor excision to thwart the cancer’s spread.
A study highlighted that India, which has a high incidence of oral cancer, often resorts to surgery as the primary treatment, with neck dissection being a common procedure for patients with clinically lymph node-negative neck.
4. Reconstructive Surgery
Following tumor removal, reconstructive surgery aims to restore both the appearance and function of the mouth. The technique employed hinges on the tumor’s size and location, ranging from skin grafts and local tissue flaps to synthetic materials.
5. Prophylactic Surgery
As a preventive measure, prophylactic surgery involves excising tissues at elevated risk of cancer manifestation. For oral cancer, this might be advised for individuals with precancerous conditions or a history of the disease to diminish recurrence chances.
6. Laser Surgery
Leveraging a concentrated beam of light, laser surgery is adept at eradicating small, surface-level tumors in the mouth or lips. Its precision ensures minimal damage to adjacent healthy tissues.
7. Palliative Surgery
For advanced oral cancer cases, palliative surgery is employed to enhance the patient’s quality of life by alleviating symptoms. The objective isn’t curing the disease but mitigating pain, swallowing difficulties, or other tumor-induced complications.
Benefits of Oral Cancer Surgery
Now that we have explored the different types of oral cancer surgery, let’s delve into the benefits mouth cancer surgery can offer:
1. Effective Removal of Cancerous Tumors
The primary objective of oral cancer surgery is to remove malignant tumors thoroughly. Surgeons employ meticulous techniques to ensure the comprehensive excision of cancer cells, thereby minimizing the risk of metastasis or spread to other body parts. Especially in the early stages of oral cancer, surgery can often be the sole treatment required to eradicate the disease, as emphasized by Healthgrades.
2. Precision in Targeting Cancer
An oral cavity cancer surgery provides the advantage of precision. Surgeons can excise tumors while inflicting minimal damage to the surrounding healthy tissues. This precision is paramount in preserving vital structures like the tongue and jaw, ensuring patients retain their ability to speak, swallow, and breathe without impediments.
3. Opportunity for Comprehensive Examination
Post-surgery, the excised tumor and adjacent tissues undergo rigorous examination to ascertain the cancer’s extent and characteristics. This data is instrumental in shaping subsequent treatment strategies. It aids in determining the necessity for adjunct therapies like radiation or chemotherapy, ensuring a holistic approach to preventing cancer recurrence.
4. Enhanced Quality of Life
Successful surgical removal of oral cancer can usher in a marked improvement in a patient’s quality of life. Eradicating the malignant growths alleviates the associated pain and discomfort, enabling individuals to regain their oral functions and savor an enhanced overall well-being.
According to Healthgrades, over 80% of patients with small, early-stage mouth cancers that haven’t metastasized are alive after five years. This statistic underscores the efficacy of surgical interventions in enhancing patient outcomes.
Risks of Oral Cancer Surgery
While oral cancer surgery is a pivotal step in treating the disease, it’s essential to be aware of the potential risks and complications associated with the procedure:
1. Surgical Complications
As with any surgery for oral cancer, there’s a risk of complications such as bleeding, infection, and adverse reactions to anesthesia. Proper post-operative care and close monitoring can help mitigate these risks.
2. Functional Impairments
Depending on the tumor’s location and the extent of the oral cavity cancer surgery, patients might experience difficulties speaking, swallowing, or breathing. For instance, tongue or throat surgeries may impact speech and swallowing functions.
3. Cosmetic Concerns
Surgical removal of tumors during oral cavity cancer surgery, especially in visible areas like the lips or face, might lead to cosmetic concerns. While reconstructive surgeries can address some of these issues, there might be permanent changes to one’s appearance.
4. Lymphedema
In cases where lymph nodes are removed during mouth cancer surgery, there’s a risk of lymphedema, which causes fluid to accumulate in the tissues, causing swelling. This is particularly relevant for surgeries that involve neck dissection.
5. Nerve Damage
There’s a potential for nerve damage during oral cancer treatment surgery, which can result in numbness, tingling, or even paralysis of certain facial muscles. For instance, nerve injuries during neck dissection can lead to ear numbness, weakness when raising the arm, or lower lip weakness, as detailed by Cancer.org.
6. Nutritional Challenges
After surgery for oral cancer, patients might face eating challenges and require a special diet or even feeding tubes for a certain period.
7. Recurrence of Cancer
While oral cancer treatment through surgery aims to remove all cancerous cells, there’s always a risk that not all cells will be removed, leading to cancer recurrence.
The Oral Cancer Surgery Process: What To Expect
Now that you learn the benefits and risks of mouth cancer surgery, it’s time to dig deep into the process to get a clear expectation of the procedure. As you consider oral cancer surgery, here’s a detailed breakdown of what the journey entails:
1. Pre-Operative Evaluation
Before embarking on the mouth cancer surgery journey, a thorough pre-operative assessment is paramount. This includes physical examinations, imaging tests, and laboratory evaluations to determine your health status and the cancer’s progression. The surgeon will provide insights into the procedure, its potential risks, and benefits, ensuring you have a clear understanding and addressing any concerns.
2. Careful Planning
At this stage, a multidisciplinary team, possibly comprising an oral surgeon and other specialists, will meticulously map out the surgery’s specifics. They’ll consider factors like the tumor’s size, its location, and the most suitable surgical technique. Additional interventions, such as neck dissection or reconstructive surgery, might also be deliberated upon.
3. Anesthesia Administration
On the oral cavity cancer surgery day, you’ll be ushered into the operating room, where anesthesia will be administered. The choice of anesthesia will be influenced by the nature of the surgery and your health profile. This will be discussed in advance to ensure you’re well-informed and comfortable.
4. Surgical Procedure
The surgical approach will differ based on the type of mouth cancer surgery being undertaken. Incisions will be made to access the tumor, which will then be meticulously removed along with any adjacent affected tissue. Your vital signs will be continuously monitored for safety.
5. Post-Operative Care
After the oral cavity cancer surgery, you’ll be under close observation in a recovery area. The duration of your hospital stay will be influenced by the surgery’s complexity and your recovery pace. Pain management and wound care will be provided. The surgical team will guide you on post-operative care and subsequent appointments.
According to Mount Sinai, post-operative care is crucial. After the oral cancer treatment, emphasis is often on reconstruction to maintain function and appearance.
Depending on the cancer’s severity, reconstruction can range from simple procedures like rejoining tongue muscles after a tongue cancer removal to more advanced procedures that might require grafting replacement skin or even transplanting tissue from other parts of your body.
Rehabilitation is also vital, especially if the oral cancer treatment has affected functions like mouth lubrication, swallowing, speech, or movement. Professionals such as speech therapists and physical therapists play a crucial role in ensuring quality of life post-surgery.
Regular follow-ups are essential not just to monitor the treated area but also to ensure no new cancers develop, especially for patients who continue to use tobacco and alcohol post-treatment.
Recovery Duration Following Mouth Cancer Surgery
The recovery period for mouth cancer surgery varies from patient to patient, depending on the extent of the procedure and individual factors. It may take several weeks to a few months to recover fully. During this time, patients may experience pain, swelling, and difficulty eating and speaking.
The recovery process after mouth cancer surgery typically involves the following:
1. Hospital Stay
A hospital stay is often necessary after mouth cancer surgery, especially for intricate procedures. This duration allows medical professionals to monitor the patient’s condition closely, manage post-surgical pain, and ensure optimal healing, as highlighted by Healthgrades.
2. Post-Operative Care
A seamless recovery hinges on meticulous post-operative care after surgery for oral cancer. This encompasses adhering to prescribed medications, adopting a specialized diet tailored to the patient’s condition, and maintaining impeccable oral hygiene.
3. Rehabilitation and Follow-Up
Post-surgery, some patients might necessitate rehabilitation services like speech or physical therapy to restore normalcy in function. Regular follow-up consultations with the oral surgeon or oncologist are paramount to tracking recovery progress and addressing emerging concerns.
Mount Sinai says post-operative care after surgery for oral cancer often emphasizes reconstruction to retain function and appearance. Rehabilitation is vital, significantly if the oral cancer treatment has impacted functions like mouth lubrication, swallowing, or speech.
4. Time for Healing
Complete recovery from the oral cavity cancer surgery might span several weeks. During this recuperative phase, it’s imperative to eschew strenuous activities and meticulously adhere to the surgeon’s directives to mitigate the risk of complications.
As per Memorial Sloan Kettering Cancer Center, the recovery process can vary based on the type of surgery and the individual’s overall health. For instance, skin grafts might necessitate a shorter recovery period, while more extensive surgeries could require a longer duration coupled with physical therapy and other rehabilitative measures.
Key Takeaway
Mouth cancer surgery is a treatment option that aims to remove cancerous tumors and affected tissues in the mouth. The recommended surgery for oral cancer varies depending on the cancer’s stage and location, and it may involve tumor excision, neck dissection, or reconstructive procedures.
Success rates for oral cancer treatment depend on various factors, including the cancer’s stage, overall health, and treatment timing. The earlier the cancer is detected, the higher the chances of successful treatment. The recovery period for mouth cancer surgery is typically a few weeks to several months, and it involves hospital stays, postoperative care, and follow-up visits.
Experience Quality Orthodontic Care From Century Dental
Are you looking for a skilled dentist in Madeira Beach, FL? Look no further than Century Dental! Our team of experienced dental professionals is committed to providing quality care and excellent customer service. Call us today to schedule an appointment!